By Katie Harris, Social Issues reporter
Original article published in NZ Herald 18th March 2022 6:00 am
WARNING: This article references mental health issues and suicide.
March is Endometriosis awareness month, a condition that effects roughly one in 10 women, and those with a uterus, in Aotearoa. Katie Harris spoke to several women about what the condition is and the difficult road some face to get support.
Wellington dancer Kanan Rei Te Maipi was 14 and in a ballet class when she first felt the intense pain.
Te Maipi knew it wasn’t normal, but every time she visited the doctor instead of helping her find the underlying issue she says she was given contraceptive pill after contraceptive pill.
None of them helped, and the 21-year-old felt the side-effects brought her down mentally and made her gain weight.
“It was just not a fun time, along with all the normal stuff that comes with being a teenager, having that [endometriosis] shoved on top was not ideal.”
It wasn’t just her doctors not listening, she says her school teachers didn’t understand what she was going through either.
“I did miss out on a lot. It actually put me in a really bad headspace with school. Teachers would wonder why I wasn’t there and then I would tell them I had cramps they would be like ‘everyone has cramps and they still come to school’.”

At 15 she was at breaking point.
“I ended up trying to take my own life because I felt like no one was listening to me and nothing was going to work for this.”
It took a chance appointment with a fill-in GP after she had fainted twice for her to finally get a referral to a gynaecologist and learn about endometriosis.
“Looking back on it now, like [with] the amount of times I went to the doctor, it baffles me that no one sent me to a gynaecologist.”
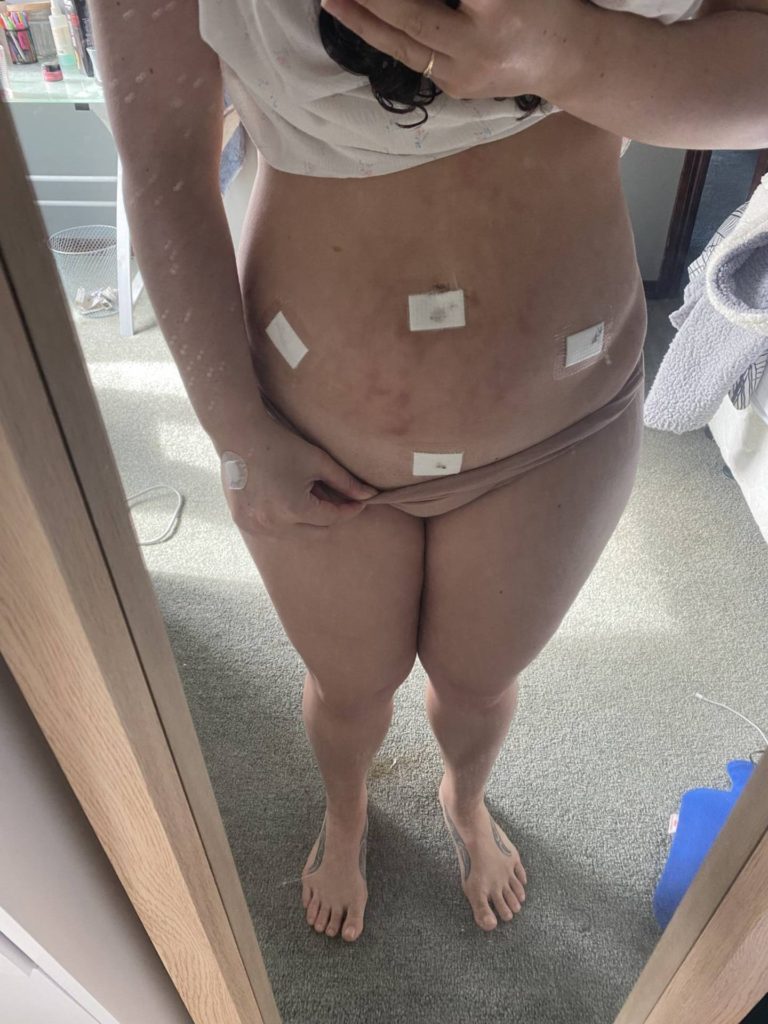
Three weeks after first seeing the gynaecologist she had a laparoscopy – the surgery needed to diagnose endometriosis.
While she was in surgery she says they discovered she had a “severe case” of endometriosis and a cyst the size of a golf ball.
“That is usually something people would be like that’s really bad, but I was like thank god I’ve got all these things. Now I’ve got all these things wrong with me and that other people can know there’s things wrong with me.”
Still, she’d spent the previous four years in agony.
Currently, there is no cure for endometriosis, however, the surgery Te Maipi had can remove the endometriosis lesions and adhesion if they are found, but in many cases, these grow back following the procedure.
Some people may also get a hysterectomy with oophorectomy (the removal of the ovaries), which is 85 per cent effective in preventing future symptoms.
Despite the years of little action by medical professionals and horrific pain, Te Maipi believes she is in a privileged position due to her mother’s insurance coverage.
This, she says, allowed her to self-refer to a gynaecologist.
“I know that there would have been people before me waiting for months and months and months just to have their surgery and I just waltzed in there.”
She believes the health system doesn’t research and fund health issues that mainly affect women as much as those that impact men.
“Even though it’s [endometriosis] something you can’t see, it doesn’t mean it isn’t real.”
Knowing that people are suffering in silence and fighting to be heard is what encourages her to keep sharing her story on her endometriosis awareness page.
“Also, for other people of colour and Māori people who, like me, have been pushed aside by the health system.
“I have friends that are white that would have been referred on their second visit to the hospital and I went over 20 times and I never got referred. I want to give people the strength to be able to speak up for themselves and to find a way to be heard.”
About 1 in 10 women have endometriosis, and the symptoms range widely from painful periods, and pain during or after sexual intercourse, mental health impacts and infertility.
Emma, who only wants to go by her first name, is still fighting for a diagnosis.
Her symptoms include cramping, painful bowel movements, waking in the middle of the night in agony, crying and being unable to walk.
“It’s like that pain that there’s nothing you can do. No position you can go helps it go away.”
It took her multiple trips to her doctor, crying in her office, to get a referral to a specialist for an ultrasound which she said happened quite quickly.
Although an ultrasound can’t diagnose endometriosis, during hers they did find a growth in her uterus called a polyp. She was told she needed to see a gynaecologist but the public waiting list was long, five months where she is, so in the meantime, Emma sought help privately.
“I paid over $300 to go and have a consultation with her. And that was really beneficial because I started understanding. We talked about the polyp and how it needs to be removed. We talked about endometriosis.”
Through this discussion, she understood she needed to have surgery but she wasn’t willing to do it privately due to the cost, which is over $10,000.
“That’s the only way that they can diagnose if you have endo, by going in through your belly button. And if they find it, they’ll take it out. If they don’t find it they’ll sew you up. So it is quite invasive surgery.”
Emma left that consultation with a script for contraception, which the gynaecologist said was because she shouldn’t be in pain, but it wasn’t the resolution she was after.
“I just have had so many horror stories from previous times I’ve been on the pill and yeah, I just I don’t think that that should be the only solution.”
A few months later she finally had an appointment with a gynaecologist in the public system who told her they would have surgery to remove her polyp growth.
However, she says he told her he wasn’t going to do a laparoscopy on her because he didn’t “feel like” her symptoms were bad enough.
“I think for him, it was like a risk factor, you know, he’s like, ‘well your pains valid I can’t tell you what you’re feeling. But the risk of us going in, and not finding in is too high and not worth it for us to do that’.”
Hearing this to her felt like he was making a judgment call on her experiences without asking what she was actually going through.
Emma says even though she detailed the impact the pain had on her life, like having to take days off work, keeping her up at night and her bowel issues he only offered her contraception options to help treat the symptoms.
Another fear weighing on her mind was the implications endometriosis could have on her fertility, to which she claims he said if she had problems with fertility in the future they would then look at doing the surgery.
“That really kind of took me by surprise, because I completely appreciate that, I know several women that have had laparoscopy, because they’ve had fertility issues. And they had endo removed. But like, what about my quality of life now? What if I never decide to have children?”
Getting support in the public system is a “long road”, she says, and those trying to find help need to push and be confident that what they’re feeling isn’t normal.
“You have to fight for yourself, no one else is gonna do it for you. I think that’s what I’ve really learned, like, this is my journey.
“Which is sad, because it shouldn’t be like that. Because there’s so many women that are experiencing the same thing, you know, you shouldn’t have to be crying in front of your doctor to get a referral.”
Herein lies the trouble for many women like Emma, as the only way to get an official diagnosis is for laparoscopy surgery, which is hard to get a public referral for.
Endometriosis New Zealand founder Deborah Bush told the Herald the diagnosis delay for endometriosis is over eight years internationally, but this varies widely.
Generally speaking, Bush says uninsured people have a much different journey with their disease than those who are insured.
A long-standing problem that she believes has been exaggerated by Covid, is that for non-cancer gynaecology referrals DHBs often have a closed-door policy.
“They often cite in their rejection letters, ‘referring back to primary care provider due to capacity issues’. It is very very common.”
She says this still occurs even if a GP has exhausted all the treatments and therapies they can do in primary care.
Bush tells the Herald she’s failed to find another illness that is so poorly managed, treated and understood as endometriosis in our system.
“It also comes down to not just capacity, but the expertise that our DHBs have to treat and manage the disease that someone may get in private practice. So it is a great anomaly, it is a terrible enigma, it’s a tragedy for those with the disease.”
For her however, the overarching problem is how early the disease starts, which can set those who have endometriosis up to have disrupted educations, interrupted development and to miss job opportunities.
She says this can have a emotional, psychosocial and mental health impacts, leading to them feeling “absolutely terrified” of getting their next periods.
“Think about these children reorganising their school lives and their friendships, and going out or going to school camps and their exams and being so panicked because that’s the time they’re having their periods.”
During this she says every day functions like going to the bathroom can be excruciatingly painful for them.
“Everyone of those people suffering has whanau, has a workplace, has those who are near and dear to her. Often she will isolate herself, and that’s when the mental health pattern comes into play.
“We are embarrassingly falling so far behind.”
Most of the people who do have suspected endometriosis in the public system won’t get a gynaecologist review in the DHBs, she says.
“They might be given opioids, and some people take these daily. And we actually know that opioids do not work for chronic pelvic pain and yet so many are on them. I know women that don’t report to ED any more, they’re so broken.”
She says it is a disgrace how people with endometriosis were being treated.

Meg Stokes, 25, doesn’t have health insurance and is also struggling to get a diagnosis.
At just 17 huge wads of skin and blood came out during her period, she says, leaving her wallowing in pain and eventually in a hospital after hours.
“Even before I get my period I’ve just got insane bloating, it’s like symptoms of IBS, but I don’t have not IBS, it’s like whenever I get my period I get real bad [gut issues].”
She describes the first three days of her menstrual cycle as “like haemorrhaging”.
“It’s just like heavy, heavy bleeding, insane PMS being really horrible to people for no reason. Having to take days off work because my period is so bad.
“And I haven’t had a definite diagnosis, like nothings confirmed.”
Stoke says up until now she hasn’t even been bothered to go on the waiting list as she says her doctor told her it will take 3.5 years.
“I really need it seen to.”
In a statement, the Ministry of Health told the Herald that delayed diagnosis can dramatically affect people’s wellbeing.
Which is why they say the Ministry launched the “Best practice guidance Diagnosis and Management of Endometriosis in New Zealand” in 2020.
“Clinical guidelines are valuable for helping to focus support from the different clinical groups involved; they help improve consistency, and also reinforce a standard approach.”
The spokesperson said the report notes that DHBs are responsible for assessing the health needs of their local populations and making decisions about the level and mix of services to provide to meet these needs.
“Patients who are referred to a DHB service are assessed and prioritised by clinicians to ensure those with the greatest need and potential to benefit from treatment receive the highest priority.”
Despite the new guidance, the Ministry noted that some referrals and waiting times in public hospitals have been extended due to the major reprioritisation of health and support services for the COVID-19 response.
“The Ministry is working closely with DHBs to support them in managing hospital treatments and increase people’s access to surgeries and consultations that may have been delayed.”



